Timing and composure are everything when it comes to emergency first aid. Composite: Guardian Design; Posed by models; Kmatta;AndreyPopov/Getty ImagesTiming and composure are everything when it comes to emergency first aid. Composite: Guardian Design; Posed by models; Kmatta;AndreyPopov/Getty ImagesHow to save a life: paramedics on emergency first aid – from cardiac arrest to burns to seizures
Timing and composure are everything when it comes to emergency first aid. Composite: Guardian Design; Posed by models; Kmatta;AndreyPopov/Getty ImagesTiming and composure are everything when it comes to emergency first aid. Composite: Guardian Design; Posed by models; Kmatta;AndreyPopov/Getty ImagesHow to save a life: paramedics on emergency first aid – from cardiac arrest to burns to seizuresWould you know how to respond if someone was taken critically ill? Experts explain the basic skills we can all learn and how to perform them with confidence
Cardiac arrest
“If you learn one thing, it should be how to resuscitate,” says Richard Webber, an associate clinical director of St John Ambulance and practising NHS paramedic in the south of England. “We know that for every one minute delay in restarting the heart, there is a 10% reduction in survivability.”
“In the UK, we have about 40,000 out-of-hospital cardiac arrests each year and the current survival rate is 9%,” says Emily Le-Gallienne, a resuscitation officer and paramedic for the East of England ambulance service, who is based in Hertfordshire. “We see much better survival rates in countries like Denmark and Sweden, because people are being taught cardiopulmonary resuscitation (CPR) skills more.” A CPR element has just been introduced to the UK driving theory test, “which is really positive progress”, says Le-Gallienne. “CPR and defibrillation can increase the chance of survival by up to 70% if it is done in the first three to five minutes of cardiac arrest, and an ambulance may not arrive in that time. If we get there and that person hasn’t received bystander CPR, what we do after is far less effective.”
Before you start CPR, call for an ambulance. It is crucial that you are sure the person is not breathing, because they could be unconscious, but not in cardiac arrest, says Oliver Siddell, a paramedic from Leeds who works for the Yorkshire ambulance service. To check, “open their airway, by tilting the head back and lifting the chin”, says Le-Gallienne. “Look at the person’s chest to see if you can see if it is rising and falling, and get really close to the person to see if you can feel any breath on your cheek. Check for a pulse if you are confident to do so. If they aren’t breathing or if their breathing is abnormal – slower, irregular or gasping – then that could be a cardiac arrest.”
 Some community defibrillators are kept in former phone boxes. Photograph: Photographer, Basak Gurbuz Derman/Getty Images
Some community defibrillators are kept in former phone boxes. Photograph: Photographer, Basak Gurbuz Derman/Getty ImagesThis is the point at which you need to perform CPR. For the chest compressions, “use the heel of the hand”, says Le-Gallienne. “Put the hands on top of each other, interlocking if it is comfortable, then push into the centre of the chest. You need to make sure that you’re doing it deep enough: for adults it is between 5cm and 6cm; for children, at least one-third of the depth of their chest, not exceeding 6cm.”
All the paramedics recommend thinking of a song to help keep the right pace (at a BPM of 100-120), such as Stayin’ Alive by the Bee Gees or Pink Pony Club by Chappell Roan. There is even a playlist on Spotify made by the British Heart Foundation, says Le-Gallienne. You should ideally do 30 chest compressions then two rescue breaths into their mouth, “but some people feel uncomfortable doing ventilations, particularly if they don’t know the person”, says Webber. If this is the case, focus on doing compressions for as long as possible: “That buys time, keeps oxygen going to the organs, and keeps the heart and brain alive.”
“If you are able to do a rescue breath,” says Araf Saddiq, a paramedic with the Scottish ambulance service who is stationed in Douglas, South Lanarkshire, “pinch the nose and open the mouth with your other hand and slowly breathe into the mouth. Wait until their chest comes back down and then breathe in once more. After the second, continue with the chest compressions.”
You can find out online where your nearest community defibrillator is, says Webber – be it at a library, community centre, or in a former phone box. You must never leave the injured person alone, so get someone else to fetch it. “Some defibrillators are in locked cabinets,” says Le-Gallienne. “The ambulance service will give you the code to unlock that cabinet.”
Saddiq says that an automated external defibrillator, the type found in public places, will literally talk you through what to do: “It has clear instructions on where the parts have to go, it will analyse the heart, and if it needs a shock, it will advise to shock. All you have to do is push a button.”
If you’re unclear about the difference between a cardiac arrest and a heart attack, the British Heart Foundation explains that “a cardiac arrest happens when your heart suddenly stops pumping blood around your body”, while “a heart attack happens when there’s a sudden loss of blood flow to a part of the heart muscle”.
Heart attack
Unlike cardiac arrest, “a heart attack is central chest pain that tends to come on suddenly”, says Webber. “People describe it as either a tight band around the chest or a vice-like grip of the chest. Pain can go up to the jaw and down the arms, more usually the left arm. In a heart attack, the heart doesn’t always stop, and you don’t need to be doing CPR, although a high proportion of people who have a heart attack then go on to have a cardiac arrest within the first hour,” says Webber. You can help someone who is having a suspected heart attack by calling for an ambulance and giving them 300mg of aspirin to chew, “because that helps to stop the clot worsening, which is what usually causes a heart attack”, says Webber. “Then, place them in a restful sitting position.”
Choking
There are clear signs that someone may be choking, says Le-Gallienne. “It could be that they are suddenly unable to speak or are coughing a lot. They may look quite flushed or point at their neck. People tend to take themselves off because they are embarrassed, especially in a public place. If you are in a restaurant and someone starts coughing, and they get up and leave the table, go and check on them.” If they are choking, call for help, says Le-Gallienne: “If it gets better without needing an ambulance, then that’s great. If it doesn’t, we should know about it as soon as possible.”
 If back blows don’t work, move on to abdominal thrusts. Photograph: Posed by models; Science Photo Library/Getty Images/Science Photo Library RF
If back blows don’t work, move on to abdominal thrusts. Photograph: Posed by models; Science Photo Library/Getty Images/Science Photo Library RFEncourage the person to cough, as that can help to dislodge whatever it is they’re choking on. If this doesn’t work, “that is when you want to start doing manoeuvres”, says Le-Gallienne. “Give up to five back blows with the heel of your hand between the shoulder blades, quite hard. If it doesn’t come out, then move to abdominal thrusts, which historically we called the Heimlich manoeuvre. Create a fist with your thumb out, and then stand behind them and pop that between the bottom of their rib cage and their belly button. Put the other hand over the top and then push in and up, almost like the shape of a letter J. Do that up to five times.” Repeat back blows and abdominal thrusts as necessary.
Drowning
Once the person is out of the water, “turn their head to let as much water out of their airway as possible”, says Le-Gallienne. “If they aren’t breathing, or are breathing abnormally, you then need to give five rescue breaths and begin CPR. With drowning it is really important that you do rescue breaths, because that person will have been without oxygen, and that will have been what caused that cardiac arrest.” Make sure the skin is dry before using a defibrillator, Le-Gallienne adds.
Severe bleeding
“We are seeing a lot more severe bleeding than 20 years ago because stabbings and shootings are more prevalent,” says Webber. If a wound is on a limb, “you can put a tourniquet 2cm to 3cm above it, tighten as much as you can and elevate it. If it is on the torso, you need to apply a dressing quite tightly and put pressure on it.”
If you don’t have a bandage, work with what you have got, says Siddell: “Not something really dirty that could put germs into the wound. If you’ve got a clean cloth or towel, that will work well. If you don’t have anything like that, you’ve just got to make the best of the situation.”
“When it comes to severed fingers or limbs,” says Saddiq, “the priority is the control of bleeding. If there is someone else there, get them to collect the finger or limb and wrap it in either clingfilm or plastic. Put it somewhere cool – but not in the freezer – or on a bag of frozen peas, so it can be reattached.”
“Don’t let the severed part touch the ice directly,” adds Webber. “If you suspect someone has broken a bone then you should avoid moving it as that can cause further damage.”
Head injury
With a bump, apply an ice pack wrapped in a tea towel to reduce swelling, says Siddell, getting help if the person seems drowsy, disoriented or is continually vomiting.
“Heads bleed quite a lot,” says Webber. “A cut to the head needs a dressing put on it to control the bleeding. A severe head injury may be a skull fracture. If the person is unconscious, you need to put them on their side and tilt the head back, or place them in the recovery position, and get help.”
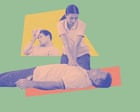
 Kneel beside the person to put them in the recovery position. Photograph: Posed by models; Johner Images/Getty Images/Johner RF
Kneel beside the person to put them in the recovery position. Photograph: Posed by models; Johner Images/Getty Images/Johner RFTo do the recovery position, “place the person on their back and check that they are unconscious but breathing normally”, says Siddell. “Kneel beside them, position the arm closest to you at a right angle, and bring their other hand across their chest to rest against their cheek. Bend the knee of the leg farthest from you, then gently roll them on to their side by pulling on that knee while keeping their hand pressed to their cheek. Tilt their head slightly back to keep the airway open, adjust the top leg so the hip and knee are at right angles, and make sure their mouth is angled downward so fluids can drain. Keep monitoring their breathing until help arrives.”
Stroke
It is vital to recognise a stroke early on, says Webber. “The mnemonic that we teach people is FAST: face, arm, speech, time. The face can droop on one side; the arms can become weak, or there’s definitely a weakness on one side compared with the other; speech can be slurred. If you notice any of these signs, it is time to call the emergency services. There is no other first aid than early recognition and calling for help.”
Burns
“Put the burnt area under a cold tap for at least 10 minutes, but ideally 20,” says Webber. “You don’t need to put anything fancy on it.” Water shouldn’t be too cold and don’t use ice, says Siddell, because that can cause more damage.
Then, cover the burn with clingfilm or a wet dressing, says Saddiq. “Don’t put a dry dressing on, because it could end up sticking to the wound.” And don’t pop any blisters: “Once a blister has been burst, it is open to infection, which could end up causing more serious problems and become septic.”
Seizures
“Don’t try to put anything in the person’s mouth, as used to be advised,” says Webber, “because the teeth can clench down. You can put something soft below their head to prevent any further injury if needed. Let them finish the seizure, make sure their airway is clear, then put them on their side or in the recovery position. If a person is not known to have seizures, if they’ve had more than one or if a seizure lasts for more than five minutes, then you must call for help.” If someone faints, “elevate their legs to the chest to help the blood return to the brain”, says Siddell.
Anaphylactic shock
“Anaphylaxis is a life-threatening allergic reaction,” says Le-Gallienne. “The mortality rate is quite low in the UK [1 in 1-3 million a year]. However, the number of people presenting with anaphylaxis is increasing.” Signs can include a change in breathing – which can often be quite noisy – a swollen tongue, wheezing, clamminess, or a loss of consciousness. “Call 999 immediately and lay the person down. Anaphylaxis can lower the blood pressure, so raise their legs if you are able to. If the person is known to have a severe allergy, they should have an adrenaline auto-injector, and it should be administered as soon as possible.”
Explore more on these topicsShareReuse this content